Video Calling Family in Nursing Homes
Amidst the COVID-19 Pandemic: Video Calling For Connecting with Family Residing in Nursing Homes
by Frank van de Baan1, MSc, Sil Aarts1,2 PhD & Hilde Verbeek1,2 PhD
1Department of Health Services Research; Care and Public Health Research Institute, Faculty of Health, Medicine and Life Sciences, Maastricht University, The Netherlands
2Living Lab in Ageing and Long-Term Care; Maastricht, The Netherlands
Introduction
Due to the SARS-CoV-2 (COVID-19) outbreak in The Netherlands, all nursing homes were closed for visitors from March to May 20201 . Consequently, while health professionals were allowed to enter nursing homes to provide care, relatives were not under any circumstances. To overcome the inability to talk to a loved one residing in a nursing home, video call technology was widely used. However, little is known regarding the experiences of relatives using this kind of technology to stay in contact with their love-one residing there. Hence, the current study was aimed at identifying the experiences of relatives of nursing home residents regarding the use of video call technology during the COVID-19 pandemic.
Methods
Data was gathered through an online questionnaire. Since long-term care facilities were not accessible due to COVID-19 protocols, a message containing information about the study and a link to the questionnaire was sent via social media. The study population included individuals that had made use of a video call program to get in contact with a person residing in a nursing home. Participation was anonymous.
Questions were formulated based on the technology acceptance model 2 (TAM2) and based on questionnaires examining the use of similar technologies in nursing homes2–5. It consisted of four main topics: (1) the perceived use of video call technology; (2) the role of nursing homes in assisting with the use of video call technology; (3) personal outcomes related to the use of video call technology; (4) future use of video call technology. Besides multiple choice questions, the questionnaire consisted questions using a 5-point Likert-scale.
Moreover, two open-ended questions were asked:
- Did the use of video calling lead to any other positive effects? And if so, which effects?
- Did the use of video calling lead to any other negative effects? And if so, which effects?
The multiple choice questions (%) and mean ratings were analysed using descriptive statistics. Compound scores were computed for statements related to the same topic. The answers to the open-ended questions were analysed using open and axial coding.
Findings
- Overall, 64 persons (78.1% female) filled in the questionnaire.
- The mean age of participants was 52.8 years (SD 14.0); for nursing home residents, the mean age was 79.6 years (SD 13.36).
- The majority of participants had a parent living in a nursing home (53.1%); the majority of relatives of participants had a form of dementia (82.8%).
- Almost all participants (93.8%) already had the technology they used themselves; 70.3% of nursing home relatives received the technology from the nursing home.
- Whatsapp was used by 51.6% of participants, followed by Skype (31.8%) and FaceTime (28.1%).
- Some participants used multiple technologies.
- In total, 85.9% of participants indicated that their relative received help from the nursing home during video calling.
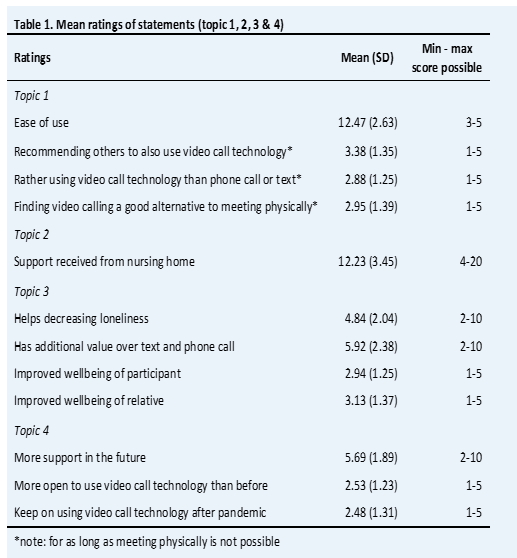 Table 1 shows the mean ratings of the statements, arranged per topic. Ratings with a min-max score other than 1-5 are compound scores. Higher scores are reflective of agreements, whereas lower scores reflect disagreement. As can be seen, participants overall agreed with the technology being easy to use. Another rating that stood out was the support received from the nursing home, which can be considered quite low.
Table 1 shows the mean ratings of the statements, arranged per topic. Ratings with a min-max score other than 1-5 are compound scores. Higher scores are reflective of agreements, whereas lower scores reflect disagreement. As can be seen, participants overall agreed with the technology being easy to use. Another rating that stood out was the support received from the nursing home, which can be considered quite low.
The analysis of the first open-ended question showed one major theme: the ability to be able to see each other while talking (see table 2 below). The answers provided to the second open-ended question identified seven themes: (1) relative not understanding video call technology, (2) emotional burden on participants, (3) missing physical contact, (4) deteriorating health status of relative (5) lack of privacy and (6) lack of support from the nursing home. While the ability to see each other was mentioned to be a positive aspect, for many the use also yielded negative effects. These included being confronted with the deteriorated health of the relative or seeing them cry. During the video call, many felt the need to comfort their relative by physically being with them, but were frustrated this was not possible.
The majority of participants did not report the support of the nursing home to be lacking. However, other participants mentioned they only were offered the ability to video call with their relative after a few weeks, which in their view was too late. In addition, in some cases the negative consequence of proper support from the nursing home during the video call seemed to be the lack of privacy caused by the fact that the nurse had to be present during the call.
Discussion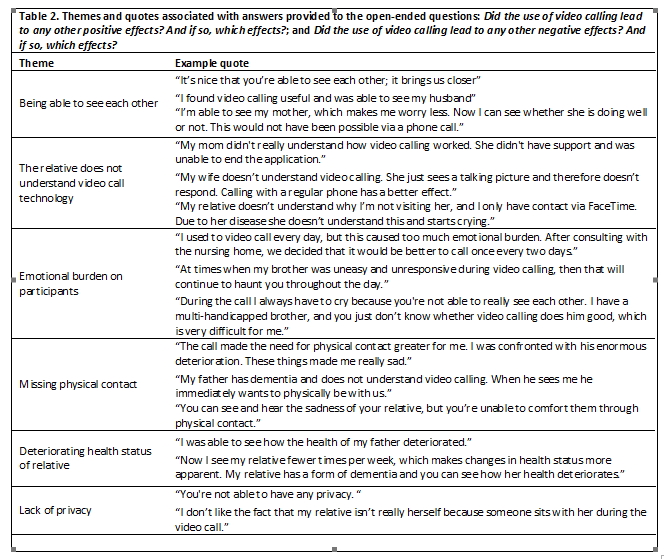
Overall, the study showed mixed results, with video call technology being more helpful for some than for others. The result of the current study also demonstrates that the cognitive ability of the relative is an important factor. Some participants reported that their relatives were unable to understand the technology due to a form of dementia. This is underscored by previous studies showing that this kind of technology isn’t a ‘one size fits all’ 6,7. Part of the unpleasant experiences of participants could also be explained by the insufficient support of the nursing home, as some participants described how the lack of support from the nursing home caused problems. Sometimes the ability to use video calling came too late (i.e. weeks after the nursing homes were closed) which led to frustration. In addition, participants reported unsolid internet connections and nurses “being digitally illiterate”. Hence, to ensure better experiences, nursing homes could ensure that their staff has the digital training needed for this type of communication and could invest in IT support. This latter option might also increase the speed with which the video call technology is introduced especially in the case of future pandemic-related restrictions. By doing so, video calling might not be a substitute for face-to-face visits, but might be a more gratifying practice.
This study had a small sample size, including participants who were already active online (and thus might already be savvy with technology). Consequently, our results should be generalized with caution. Qualitative studies could be conducted to provide more in-depth insights into experiences regarding video call technology and the support of the nursing home. These could then also focus on how relatives view other alternatives to physical contact.
References
- Verbeek, H. et al. J Am Med Dir Assoc. 21: 900-904, 2020.
- Cotten, S. et al. J Med Internet Res. 2: 1-13, 2013.
- Holden, R. J. et al. J Biomed Inform. 1: 159-172.
- Pai, F. et al. Technol Forecast Soc Change. 4: 650-660.
- Wong, A. et al. PLoS ONE. 8: 1-7.
- Mickus, M. et al. Aging Ment Health. 4: 387-396.
- Zamir, S. et al. BMC Geriatr. 1: 1-13.
Frank van de Baan is a Health Scientist and conducted this research for his Master Thesis within the specialization of Healthcare Policy, Innovation and Management at Maastricht University, The Netherlands
Dr. Sil Aarts is a psychologist and her area of expertise includes technology and data science in long-term care.
Prof. dr. Hilde Verbeek is a psychologist whose research focuses at long-term care environments for older people. She is the vice-chair of the Living Lab in Ageing and Long-Term Care in the Netherlands, an interdisciplinary partnership between 7 long-term care organizations, 2 vocational training institutes, Zuyd University of Applied Sciences and Maastricht University.









